Your digestive wellness is within reach.
Experience relief and revitalisation with specialised gastrointestinal care
provided by independent specialists and healthcare professionals.
Often, vomiting is a natural response that our bodies experience when trying to expel harmful substances and microorganisms from the stomach. However, if you find that your vomiting episodes are persistent with a specific colour, you may suffer from an underlying medical condition.
In this guide, the Centre for Gastrointestinal Health breaks down the different colours of vomit, their meanings and what they could signal about your health.
Commonly, the colour of your vomit comes from food or beverages consumed before you start feeling ill. Additionally, the distinct shade of your vomit depends on other factors such as:
Although not a decisive factor, the colour of your vomit can also provide insight into the potential cause of your illness or the specific stage of an underlying medical condition. From gut infections such as food poisoning to internal bleeding in the digestive tract, various health complications can also influence the colour of our vomit.
Therefore, it is important to take note of our vomit colour to understand what is happening inside our bodies.
You may notice that your vomit can come in varying shades, colours and forms. Such colours can include:
Below is a colour chart explaining the different medical conditions that could influence your vomit’s specific appearance.
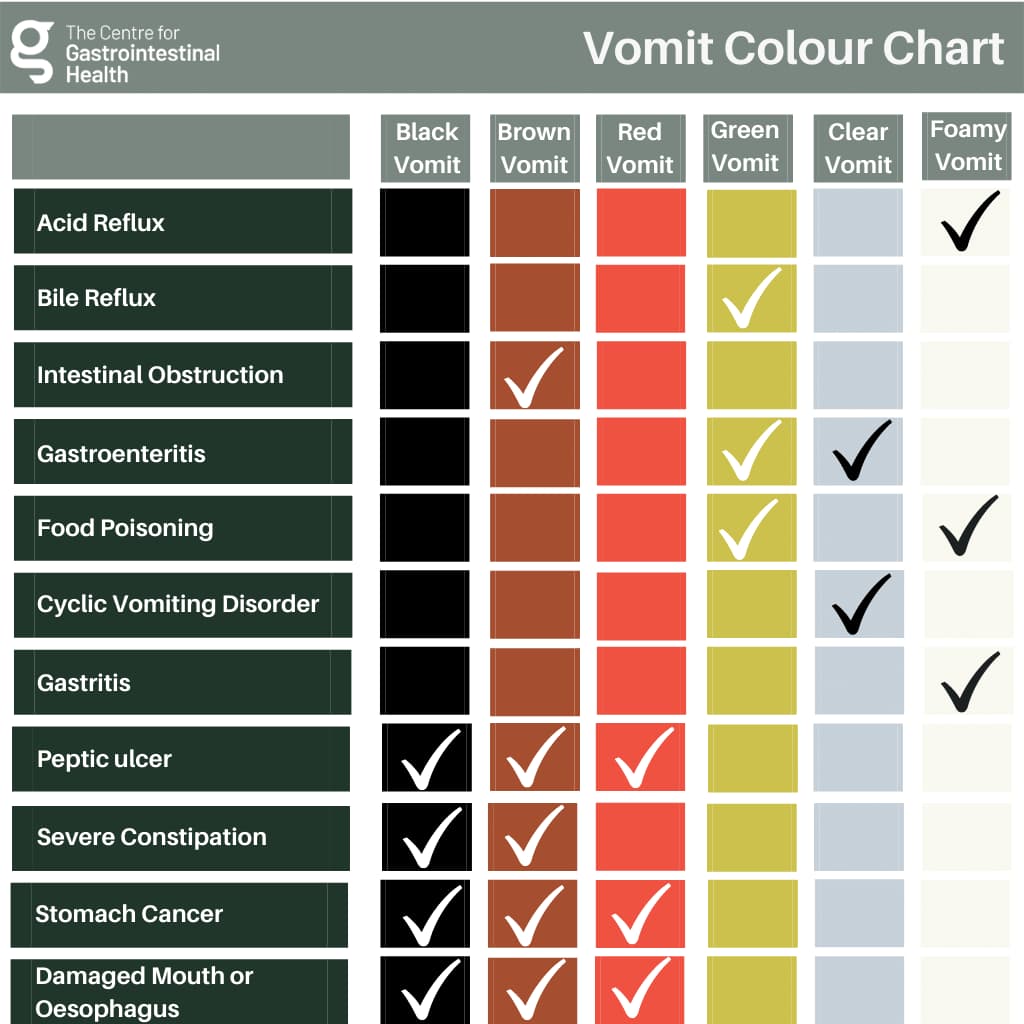
Black vomit, also known as coffee ground emesis or coffee ground vomitus, is a colour that signals several underlying medical causes. The dark colour is due to partially digested blood which causes the vomit to appear black or similar to coffee grounds.
Therefore, black vomit typically suggests some form of internal bleeding.
Some causes of black vomit include:
People who are at particular risk of these conditions include those who take Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) or suffer from late stages of kidney disease, liver disease, and certain blood clotting disorders.
Furthermore, people who struggle with alcohol abuse that may suffer from liver failure are also at risk. This is particularly relevant if you vomit black after drinking alcohol.
As black vomit is connected to several serious conditions, we consider the colour a cause for concern and, therefore, will require medical intervention.
Before alarming yourself, it is first important to reflect on what you consumed before feeling ill, as this could be a logical explanation behind the abnormal colour.
However, you should seek immediate medical attention if you’re frequently vomiting and experiencing symptoms such as severe chest pain, abdominal pain and fainting. ‘
Treatments will vary depending on the specific underlying cause of your black vomiting. During the diagnosis, a doctor will need to assess the location of the internal bleeding through an upper endoscopy or stool sample.
Following this, doctors may prescribe medication such as proton pump inhibitors which minimises the production of digestive fluids like stomach acid. In extreme cases of internal bleeding, you may need to undergo surgery.
Similar to black vomit, brown vomit can look like a lighter shade of coffee grounds with a slightly lumpy texture.
Brown vomit is often no cause for concern, with many cases coming from people eating too many chocolate-based foods. However, if you are vomiting brown on an empty stomach, it could indicate a cause for concern.
Aside from an excessive intake of food coloured brown, there are two potential causes for this type of vomit:
Common symptoms of these two conditions include severe abdominal pain, bloating and stomach cramping.
You should consult a medical professional if you are experiencing symptoms similar to severe constipation or internal bleeding.
Similar to treatment for black vomit, you will need to undergo a range of examinations to confirm the location of internal bleeding (if present). Following this, you may be prescribed medications or be required to undergo surgery.
In the case of extreme constipation, a doctor may advise you to increase your fluid intake, eat fibrous foods, and prescribe laxatives to help promote bowel movements.
Where black or dark brown vomit indicates partially digested blood, red and pink vomit flags the presence of fresh blood.
If you have found yourself vomiting large amounts of red or pink vomit, you must seek medical attention urgently, as this could be a life-threatening emergency.
Some common causes that could be causing your bloody vomit include:
Like always, you must reflect on your recent meals within a 24-hour window to assess if any substances could influence your red or pink coloured vomit.
If you believe your red vomit results from the conditions listed above, you should consult a doctor as soon as possible. An emergency hospital assessment will confirm a diagnosis and ensure proper personalised treatment for your ill health.
If you are vomiting a green or yellow substance, there is no cause for alarm. This is because green or yellow vomit indicates short-term illnesses that are not considered medical emergencies.
Depending on the specific cause, yellow or green vomit lasts for less than 48 hours unless you suffer from chronic conditions such as cyclic vomiting disorder or inflammatory bowel disease (IBD).
You may notice your vomit is green or yellow if you have an empty stomach. This is because there is no partially digested food mixed with liquids such as bile.
Bile is a greenish-yellow type of special digestive liquid that causes your vomit to change colour when there is no presence of food in the stomach. Therefore, this causes your vomit to present as a green or yellow colour.
Some common causes where this process occurs include:
While most of these conditions are not life-threatening, it is still important to seek medical assistance if your symptoms persist for more than 48 hours.
Depending on the cause, you can expect several treatments to help manage your yellow or green vomit. For instance, if you’re suffering from food poisoning, your doctor may recommend maintaining a high fluid intake to help your body recover naturally.
In the instance where you’re suffering from gastroenteritis, your doctor may prescribe a series of antibiotics or antacids to help overcome the infection. Meanwhile, treatment for bile reflux may include a few lifestyle changes, and bowel obstruction may require a more hands-on approach.
Clear vomiting is most common when the stomach has no contents to expel, including bile. Therefore, with minimal contents to regurgitate, your vomit will appear clear with no specific colouring.
Your vomit may be clear if you have been experiencing a severe episode of throwing up, consequently leaving your body with no more contents to regurgitate.
This is common in people who have:
These illnesses shouldn’t last for more than a couple of days. However, you should consult a doctor if your vomiting persists for more than 48 hours and you are experiencing symptoms such as fever, weight loss, bloating or other flu-like symptoms.
Your doctor may prescribe you a series of antibiotics or anti-nausea pills to help you keep food and liquids down. In the meantime, if you find that your clear vomit occurs after drinking water, try taking small sips and stick to bland-tasting foods.
We recommend that you always talk to a doctor before taking over-the-counter medications, especially if you are pregnant and experiencing morning sickness.
A foamy or white vomit is most common among patients who have excess gas or are experiencing acid reflux. It is important to note what food or drinks you consumed before throwing up a foamy white liquid, as dairy products or fizzy drinks can produce a similar consistency.
Your white and foamy vomit may be a result of:
If you believe that your white foamy vomit results from either of these conditions, we suggest you consult a doctor for treatment.
Treatment is essential for both these conditions to avoid further damage to your body. In the case where gastritis or GORD is causing your white foamy vomit, a doctor may recommend lifestyle changes such as reducing alcohol intake and avoiding spicy foods. Your doctor may also prescribe proton-pump inhibitors to neutralise your stomach acid if you are experiencing chronic reflux.
Meanwhile, if your white foamy vomit results from a hernia, you will require non-invasive surgery. Head to our service page for more information on our hernia surgery options.
If you are vomiting an abnormal colour for more than 48 hours, we recommend consulting a gastroenterologist for an examination. At the Centre for Gastrointestinal Health, we are experts in determining the underlying causes of your vomiting to ensure personalised and targeted treatment.
For more information on our services, call us today at 1300 580 239 or book an appointment online by filling out our contact form.
Experience relief and revitalisation with specialised gastrointestinal care
provided by independent specialists and healthcare professionals.